WHY ARE PEOPLE ENROLLING?
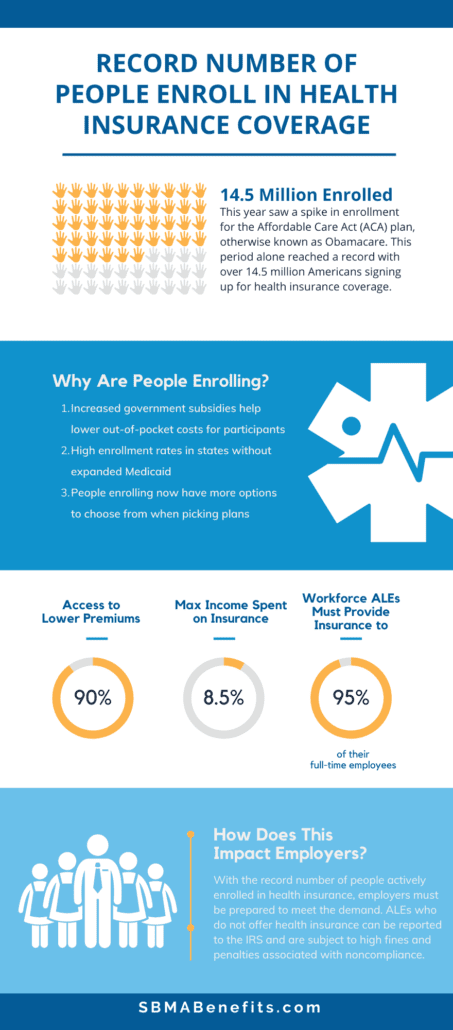
Advisors attribute this surge in registration to increased government subsidies that help lower out-of-pocket costs for participants. In fact, 90% of health insurance consumers under the ACA had access to lower premiums.
For now, those enrolling in health insurance do not pay more than 8.5% of their income towards insurance coverage—which now includes individuals at or above 400% of the FLP.
The last surge happened in 2016 when we saw 12.7 million people enroll. CNN found that currently, “roughly 27 million Americans are still uninsured, and 64% of them are eligible for coverage assistance.” If the Biden Administration’s Build Back Better bill passes both the House of Representatives and the Senate, subsidies and expansions from the American Rescue Plan will continue for those ensured in Obamacare through 2025.
Xavier Becerra, Secretary of Health and Human Services, attributes the spike in enrollment to “delivering on [their] commitment to mak[ing] healthcare a right for Americans and to ensure it is accessible and affordable.”
The next few years may see continuous surges in health insurance enrollment as people search for affordable health coverage. If the bill does not pass, however, the benefits tied into the bill will not either.
States with the highest enrollment include Florida, Georgia, and Texas. High enrollment rates here are due largely in part because these states have not expanded Medicaid.
KHN explains that “in expansion states, people with incomes from 100%-138% of the federal poverty level can enroll in Medicaid. In states that haven’t expanded the program, they can get subsidies to enroll in private plans through [ACA] marketplaces.”
More than ever before, people have access to healthcare coverage with lower premiums. A recent poll from the Kaiser Family Foundation shows public support for Obamacare at an all-time high. The ACA is gaining widespread popularity.
People enrolling now also have more options to choose from when selecting plans. The marketplace now offers up to seven different options whereas previous years provided only about four different insurers to choose from.